Items filtered by date: April 2025
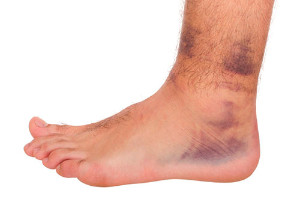
Three Types of Ankle Sprains
Research has indicated the chances of a full recovery from an ankle sprain may be increased when an aggressive role in healing is practiced after the injury occurs. This may include initially wrapping the affected ankle in an elastic bandage followed by performing gentle stretching techniques when the ankle begins to feel better. These practices may help the ankle to heal faster which can be beneficial in resuming any sporting activity. There are known to be three types of ankle sprains. Light sprains will generally heal in approximately three weeks. If the ligaments are severely stretched, recovery may last between four and six weeks. Torn ligaments are referred to as a serious ankle sprain, and the healing process can take up to three months. If you have endured an ankle sprain, it is advised that you speak to a podiatrist who can properly treat this condition.
Ankle sprains are common but need immediate attention. If you need your feet checked, contact Dr. Ronald Sheppard from Warren-Watchung Podiatry Center. Our doctor can provide the care you need to keep you pain-free and on your feet.
How Does an Ankle Sprain Occur?
Ankle sprains take place when the ligaments in your ankle are torn or stretched beyond their limits. There are multiple ways that the ankle can become injured, including twisting or rolling over onto your ankle, putting undue stress on it, or causing trauma to the ankle itself.
What Are the Symptoms?
- Mild to moderate bruising
- Limited mobility
- Swelling
- Discoloration of the skin (depending on severity)
Preventing a Sprain
- Wearing appropriate shoes for the occasion
- Stretching before exercises and sports
- Knowing your limits
Treatment of a Sprain
Treatment of a sprain depends on the severity. Many times, people are told to rest and remain off their feet completely, while others are given an air cast. If the sprain is very severe, surgery may be required.
If you have suffered an ankle sprain previously, you may want to consider additional support such as a brace and regular exercises to strengthen the ankle.
If you have any questions please feel free to contact one of our offices located in Marlboro and Watchung, NJ . We offer the newest diagnostic and treatment technologies for all your foot and ankle needs.
Rheumatoid Arthritis in the Feet
Although rheumatoid arthritis attacks multiple bones and joints throughout the entire body, ninety percent of people who actually develop this condition usually do so in the foot or ankle area. Those who develop this kind of arthritis in the feet usually develop symptoms around the toes and forefeet first, before anywhere else. Rheumatoid arthritis appears to have a genetic component. If it runs in the family, then you will be more likely to develop it as well.
Rheumatoid arthritis is an autoimmune disorder in which the body’s own immune system attacks the lining of the membranes surrounding the joints. This causes inflammation of the membrane lining, and the gradual destruction of the joint’s cartilage and even bone.
Some of the most common symptoms that are associated with RA include pain and swelling of the feet. Stiffness in the feet is also another common symptom that people experience. Those who have RA in the feet usually feel the pain in the ball or sole of their feet. This can get to be very painful at times. A person's joints can even shift and become deformed after a period of time.
In order to properly diagnose RA in the feet it is usually necessary for a doctor or podiatrist to evaluate the area. Your doctor will also question you about your medical history, occupation, etc., to determine whether anything in your lifestyle may have triggered the condition. There are a number of tests that may be performed to help diagnose RA, such as a rheumatoid factor test. There is, however, no one single test that will tell you for sure if you have RA. There are different X-rays that can be taken as well to determine if a person has RA in their feet.
There is a range of treatment options for rheumatoid arthritis. Treatment of RA is usually a lifelong process that includes a variety of methods of treatment and therapy. Your doctor can prescribe special shoes that should help with arch support as well as heel support. A physical therapist can help those with this condition learn exercises which will keep their joints flexible. Surgery may be needed to correct some of the issues with the feet, such as bunions, and hammertoes. Fusion is usually the most successful surgical option for rheumatoid arthritis. However, people need to keep in mind that there are some risks associated with these surgeries.
Impacts of Rheumatoid Arthritis on the Feet
 Rheumatoid Arthritis, or RA for short, may develop when your immune system attacks your joint lining tissue, causing painful inflammation and stiffness. To help detect if this condition is affecting you, note the following symptoms: pain or stiffness in the toe joints, aching or soreness in the feet after regular activity such as walking or standing for long periods of time, and swelling in your toe joints or ankles. To help relieve these symptoms, it is advised to wear open-toed shoes, get regular sleep, quit smoking, reduce stress, and keep your joints warm. It is important to note that symptoms don’t always show up right away, which is why it is recommended that you see a podiatrist for a proper diagnosis and advised recovery regime.
Rheumatoid Arthritis, or RA for short, may develop when your immune system attacks your joint lining tissue, causing painful inflammation and stiffness. To help detect if this condition is affecting you, note the following symptoms: pain or stiffness in the toe joints, aching or soreness in the feet after regular activity such as walking or standing for long periods of time, and swelling in your toe joints or ankles. To help relieve these symptoms, it is advised to wear open-toed shoes, get regular sleep, quit smoking, reduce stress, and keep your joints warm. It is important to note that symptoms don’t always show up right away, which is why it is recommended that you see a podiatrist for a proper diagnosis and advised recovery regime.
Because RA affects more than just your joints, including the joints in your feet and ankles, it is important to seek early diagnosis from your podiatrist if you feel like the pain in your feet might be caused by RA. For more information, contact Dr. Ronald Sheppard of Warren-Watchung Podiatry Center. Our doctor will assist you with all of your podiatric concerns.
What Is Rheumatoid Arthritis?
Rheumatoid Arthritis (RA) is an autoimmune disorder in which the body’s own immune system attacks the membranes surrounding the joints. Inflammation of the lining and eventually the destruction of the joint’s cartilage and bone occur, causing severe pain and immobility.
Rheumatoid Arthritis of the Feet
Although RA usually attacks multiple bones and joints throughout the entire body, almost 90 percent of cases result in pain in the foot or ankle area.
Symptoms
- Swelling and pain in the feet
- Stiffness in the feet
- Pain on the ball or sole of feet
- Joint shift and deformation
Diagnosis
Quick diagnosis of RA in the feet is important so that the podiatrist can treat the area effectively. Your doctor will ask you about your medical history, occupation, and lifestyle to determine the origin of the condition. Rheumatoid Factor tests help to determine if someone is affected by the disease.
If you have any questions please feel free to contact one of our offices located in Marlboro and Watchung, NJ . We offer the newest diagnostic and treatment technologies for all your foot and ankle needs.
Why Live with Pain and Numbness in Your Feet?
Morton's Neuroma
A neuroma is a thickening of nerve tissue and can develop throughout the body. In the foot, the most common neuroma is a Morton’s neuroma; this typically forms between the third and fourth toes. The thickening of the nerve is typically caused by compression and irritation of the nerve; this thickening can in turn cause enlargement and, in some cases, nerve damage.
Neuromas can be caused by anything that causes compression or irritation of the nerve. A common cause is wearing shoes with tapered toe boxes or high heels that force the toes into the toe boxes. Physical activities that involve repeated pressure to the foot, such as running or basketball, can also create neuromas. Those with foot deformities, such as bunions, hammertoes, or flatfeet, are more likely to develop the condition.
Symptoms of Morton’s neuroma include tingling, burning, numbness, pain, and the feeling that either something is inside the ball of the foot or that something in one’s shoe or sock is bunched up. Symptoms typically begin gradually and can even go away temporarily by removing one’s shoes or massaging the foot. An increase in the intensity of symptoms correlates with the increasing growth of the neuroma.
Treatment for Morton’s neuroma can vary between patients and the severity of the condition. For mild to moderate cases, padding, icing, orthotics, activity modifications, shoe modifications, medications, and injection therapy may be suggested or prescribed. Patients who have not responded successfully to less invasive treatments may require surgery to properly treat their condition. The severity of your condition will determine the procedure performed and the length of recovery afterwards.
What Causes Morton’s Neuroma?
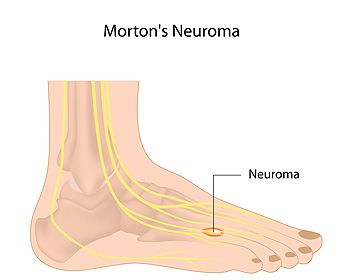 Patients who have pain and discomfort in between the third and fourth toes may have a condition that is referred to as Morton’s Neuroma. Additionally, pain can be felt on the on the ball of the foot, and under the toes. This condition is defined as a thickening of nerve tissue, and can cause a sharp, burning pain. A common reason why this ailment may develop can be connected to wearing high heels. This may be a result of not having ample room for the toes to move freely in. Moderate relief may be obtained if lower-heeled shoes are worn. If existing medical conditions are present such as hammertoes or bunions, the likelihood may increase for Morton’s neuroma to develop. After a diagnosis is performed, which typically includes having an X-ray, ultrasound, or MRI taken, the correct treatment process can begin. It is strongly advised to discuss your symptoms with a podiatrist who can offer you correct methods to manage this ailment.
Patients who have pain and discomfort in between the third and fourth toes may have a condition that is referred to as Morton’s Neuroma. Additionally, pain can be felt on the on the ball of the foot, and under the toes. This condition is defined as a thickening of nerve tissue, and can cause a sharp, burning pain. A common reason why this ailment may develop can be connected to wearing high heels. This may be a result of not having ample room for the toes to move freely in. Moderate relief may be obtained if lower-heeled shoes are worn. If existing medical conditions are present such as hammertoes or bunions, the likelihood may increase for Morton’s neuroma to develop. After a diagnosis is performed, which typically includes having an X-ray, ultrasound, or MRI taken, the correct treatment process can begin. It is strongly advised to discuss your symptoms with a podiatrist who can offer you correct methods to manage this ailment.
Morton’s neuroma is a very uncomfortable condition to live with. If you think you have Morton’s neuroma, contact Dr. Ronald Sheppard of Warren-Watchung Podiatry Center. Our doctor will attend to all of your foot care needs and answer any of your related questions.
Morton’s Neuroma
Morton's neuroma is a painful foot condition that commonly affects the areas between the second and third or third and fourth toe, although other areas of the foot are also susceptible. Morton’s neuroma is caused by an inflamed nerve in the foot that is being squeezed and aggravated by surrounding bones.
What Increases the Chances of Having Morton’s Neuroma?
- Ill-fitting high heels or shoes that add pressure to the toe or foot
- Jogging, running or any sport that involves constant impact to the foot
- Flat feet, bunions, and any other foot deformities
Morton’s neuroma is a very treatable condition. Orthotics and shoe inserts can often be used to alleviate the pain on the forefront of the feet. In more severe cases, corticosteroids can also be prescribed. In order to figure out the best treatment for your neuroma, it’s recommended to seek the care of a podiatrist who can diagnose your condition and provide different treatment options.
If you have any questions, please feel free to contact one of our offices located in Marlboro and Watchung, NJ . We offer the newest diagnostic and treatment technologies for all your foot care needs.
Treating Toenail Fungus
Fungal infection of the toenail, or onychomycosis, typically appears as a gradual change in a toenail’s texture and color that involves brittleness and darkening. The fungal infection itself occurs beneath the surface of the nail. Aside from discoloration, other symptoms include the collection of debris beneath the nail plate, white marks on the nail plate, and a foul odor emanating from the nail. If ignored, the infection can spread into other nails and the skin; in severe cases, it can hinder one’s ability to work or walk.
The toenails are particularly vulnerable to contracting infection in moist environments where people are likely to be walking barefoot, such as around swimming pools, public showers, and locker rooms. Fungal infection may also be more likely to occur in nail beds that have been injured, and sufferers of chronic diseases such as diabetes, circulatory problems, or immunodeficiency conditions are particularly prone to developing fungal nails.
Fungal nails can be primarily prevented by practicing proper hygiene and regularly examining the feet and toes. Carefully washing the feet with soap and water and thoroughly drying the feet afterwards are essential. Other tips include wearing shower shoes in public areas, changing shoes and socks daily, keeping toenails clipped at a short length, wearing breathable shoes that fit properly, wearing moisture-wicking socks, and disinfecting home pedicure tools and instruments used to cut nails.
Fungal nail treatment may vary between patients and the severity of the condition. Your podiatrist may suggest a daily routine of cleansing that spans over a period of time to ease mild infections. Over-the-counter or prescription antifungal agents may also be prescribed, including topical and/or oral medications. Debridement, or the removal of diseased nail matter and debris, may also be performed. In more severe cases, surgical treatment may be needed. In some instances, the temporary removal of the fungal nail allows for the direct application of a topical antifungal to the nail bed. In other cases, a chronically painful fungal nail that has not responded to other treatments may be permanently removed; this allows the infection to be cured and avoids the growth of a deformed nail.
Toenail Fungus Can Become Severe
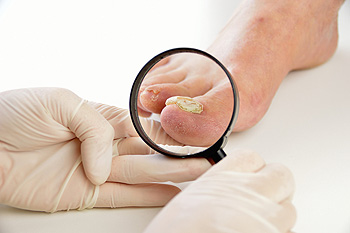 A common condition that many patients suffer from is known as toenail fungus. There are noticeable symptoms that exist with this condition and they often consist of yellowed and thickened toenails. In severe cases, the nail may separate from the nail bed, and can eventually fall off. It is caused by a fungus that lives and thrives in moist environments. These areas can include public swimming areas, shower room floors, and locker rooms. It is considered to be contagious, and measures can be implemented that may help in preventing this condition. These can consist of wearing appropriate shoes while in these types of places, and it is helpful to avoid sharing towels and shoes. There are several treatment methods that can be used for toenail fungus, and it is advised to consult with a podiatrist who can provide the best options for you.
A common condition that many patients suffer from is known as toenail fungus. There are noticeable symptoms that exist with this condition and they often consist of yellowed and thickened toenails. In severe cases, the nail may separate from the nail bed, and can eventually fall off. It is caused by a fungus that lives and thrives in moist environments. These areas can include public swimming areas, shower room floors, and locker rooms. It is considered to be contagious, and measures can be implemented that may help in preventing this condition. These can consist of wearing appropriate shoes while in these types of places, and it is helpful to avoid sharing towels and shoes. There are several treatment methods that can be used for toenail fungus, and it is advised to consult with a podiatrist who can provide the best options for you.
If left untreated, toenail fungus may spread to other toenails, skin, or even fingernails. If you suspect you have toenail fungus it is important to seek treatment right away. For more information about treatment, contact Dr. Ronald Sheppard of Warren-Watchung Podiatry Center. Our doctor can provide the care you need to keep you pain-free and on your feet.
Symptoms
- Warped or oddly shaped nails
- Yellowish nails
- Loose/separated nail
- Buildup of bits and pieces of nail fragments under the nail
- Brittle, broken, thickened nail
Treatment
If self-care strategies and over-the-counter medications does not help your fungus, your podiatrist may give you a prescription drug instead. Even if you find relief from your toenail fungus symptoms, you may experience a repeat infection in the future.
Prevention
In order to prevent getting toenail fungus in the future, you should always make sure to wash your feet with soap and water. After washing, it is important to dry your feet thoroughly especially in between the toes. When trimming your toenails, be sure to trim straight across instead of in a rounded shape. It is crucial not to cover up discolored nails with nail polish because that will prevent your nail from being able to “breathe”.
In some cases, surgical procedure may be needed to remove the toenail fungus. Consult with your podiatrist about the best treatment options for your case of toenail fungus.
If you have any questions, please feel free to contact one of our offices located in Marlboro and Watchung, NJ . We offer the newest diagnostic and treatment technologies for all your foot care needs.
Causes, Symptoms, and Treatment of Poor Blood Circulation in the Feet
Poor blood circulation in the feet and legs is often caused by peripheral artery disease (PAD), which is usually the result of a buildup of plaque in the arteries. Plaque buildup, or atherosclerosis, can be the result of excess calcium and cholesterol in the bloodstream. This restricts how much blood can flow through arteries. Reduced blood flow to a certain area of the body severely limits the amount of oxygen and nutrients that part of the body receives. This leads to degeneration in the muscles and other tissues. Sometimes, poor blood circulation in the feet and legs can be caused by other conditions, such as the damaging or inflammation of blood vessels, known as vasculitis.
The lack of oxygen and nutrients caused by poor blood circulation can restrict muscle growth and development, as well as cause muscle pain and cramps, weakness, and stiffness. Other common symptoms include numbness in the legs and feet, skin discoloration in the affected limbs, slower nail and hair growth, and erectile dysfunction in men. In more severe cases of PAD, pain can be present even when a person isn't exercising, and may range from mildly uncomfortable to completely debilitating.
Poor blood circulation in the feet and legs is more common in those who are overweight or obese, have diabetes, high blood pressure, high cholesterol, who smoke, or who have a family history of PAD or related conditions such as a heart attack, stroke, etc. Diabetes and smoking place a person at greatest risk for developing poor blood circulation, although advanced age, over 50, can also increase risk.
If you are experiencing poor blood circulation in the feet and legs caused by PAD, it is important to make changes to your lifestyle in order to reduce your risk of experiencing a heart attack or stroke caused by this condition. If you smoke, quit completely. This will increase the amount of oxygen in your bloodstream. Exercising and reducing the saturated fats in your diet. Saturated fats come from fatty meats, fried foods, whole milk, etc., can make a difference in improving blood circulation in feet. It is also important to avoid developing influenza and to carefully control your blood sugar if you have diabetes.
Your doctor may recommend combining lifestyle changes with a prescription medication regimen to improve blood circulation. The most commonly-used medications for PAD are called statins and work by blocking the amount of enzymes in your body that produce cholesterol. They are known by the brand names Zocor, Lipitor, Crestor, and others.
Possible Causes of Poor Circulation
 Research has indicated that if you have poor circulation in your feet, it may be indicative of other medical conditions. These may include diabetes, heart conditions, and obesity. It is defined as restricted blood flow to the lower extremities, and there are often noticeable symptoms that are associated with this condition. These can consist of numbness, tingling, and muscle cramps, in addition to pain and discomfort. Nerve damage can possibly be caused by poor circulation, in addition to varicose veins and blood clots. Patients may find relief when specific exercises are performed, and compression stockings are worn that are designed for painful, swollen legs. If you feel you have symptoms of this condition, it is advised that you consult with a podiatrist to learn about the best treatment options for you.
Research has indicated that if you have poor circulation in your feet, it may be indicative of other medical conditions. These may include diabetes, heart conditions, and obesity. It is defined as restricted blood flow to the lower extremities, and there are often noticeable symptoms that are associated with this condition. These can consist of numbness, tingling, and muscle cramps, in addition to pain and discomfort. Nerve damage can possibly be caused by poor circulation, in addition to varicose veins and blood clots. Patients may find relief when specific exercises are performed, and compression stockings are worn that are designed for painful, swollen legs. If you feel you have symptoms of this condition, it is advised that you consult with a podiatrist to learn about the best treatment options for you.
While poor circulation itself isn’t a condition; it is a symptom of another underlying health condition you may have. If you have any concerns with poor circulation in your feet contact Dr. Ronald Sheppard of Warren-Watchung Podiatry Center. Our doctor will treat your foot and ankle needs.
Poor Circulation in the Feet
Peripheral artery disease (PAD) can potentially lead to poor circulation in the lower extremities. PAD is a condition that causes the blood vessels and arteries to narrow. In a linked condition called atherosclerosis, the arteries stiffen up due to a buildup of plaque in the arteries and blood vessels. These two conditions can cause a decrease in the amount of blood that flows to your extremities, therefore resulting in pain.
Symptoms
Some of the most common symptoms of poor circulation are:
- Numbness
- Tingling
- Throbbing or stinging pain in limbs
- Pain
- Muscle Cramps
Treatment for poor circulation often depends on the underlying condition that causes it. Methods for treatment may include insulin for diabetes, special exercise programs, surgery for varicose veins, or compression socks for swollen legs.
As always, see a podiatrist as he or she will assist in finding a regimen that suits you. A podiatrist can also prescribe you any needed medication.
If you have any questions, please feel free to contact one of our offices located in Marlboro and Watchung, NJ . We offer the newest diagnostic and treatment technologies for all your foot care needs.